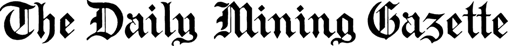COVID-19 testing:Why you haven’t been given a COVID-19 test yet

Carlos Osorio/AP Photo Examination tents are setup at the Michigan State Fairgrounds, Friday, March 27, in Detroit, where the city is preparing for coronavirus drive up testing. Even if tests become widely available, widespread community testing is not likely in most of the country.
A negative COVID-19 test result would be comforting for those sheltering at home or still going to work during the stay home order, but tests have not been readily available, and even those samples taken are not being processed very quickly. Test availability is being expanded as quickly as possible, but even once they are widely available, there are reasons to expect you may not be offered one.
TEST AVAILABILITY
While the medical community is facing a variety of equipment and supply shortages during the current pandemic, one that is limiting tests in particular is the lack of a substance used in the testing process. This is what test swabs are put into for their trip to the test lab.
“It’s called a viral transport media,” Claire Danielson said. “It preserves it (the sample).”
Danielson is a Medical Lab Scientist who teaches medical lab instrumentation at MTU.
Depending on the equipment being used, there are other supplies like test cartridges that are also in short supply, she said.
The other issue is that labs can’t just immediately start performing tests because they have the supplies. They have to check that their equipment and supplies give the same results using test samples with known values. This is called a validation study, and it can take some time.
“Just to make sure that whatever equipment we’re using is putting out accurate results,” Danielson said.
Once the equipment is validated, a single test can take as long as an hour.
“Every test is not the same,” Danielson said.
Some tests are ready in minutes, other machines can process multiple samples, but take much longer, and new tests are being developed, too. But hospitals and health departments are limited by their locally-held equipment and supplies for now.
Danielson said that many tests are regularly sent to large commercial labs around the country. Those labs, similarly limited in testing capacity, are prioritizing tests from hotspots like New York and California right now, leaving rural areas to rely on smaller, local labs.
POSITIVE PREDICTIVE VALUE
When testing members of the public, doctors have to consider something called “positive predictive value,” explained Kelly Kamm.
“Positive predictive value is the probability that, if you test positive, what is the likelihood that you actually have the disease?” she said in an email.
Kamm is an epidemiologist who teaches at Michigan Technological University. One of her focuses is rural health and social determinants of health.
“When we develop new tests for diseases, we have measures of sensitivity and specificity,” Kamm said.
Sensitivity is how likely the test is to show a positive result for someone who has the disease. Specificity is how likely the test is to show a negative result for someone who does not have the disease. You want both of these to be high, but test developers need to strike a balance between the two.
“As one goes up, the other goes down,” Kamm said.
So the developer has to decide if it is more important to catch more positive cases, or to avoid giving a false positive.
“Given the situation of COVID-19, we want to make sure we identify as many cases as possible in order to interrupt transmission,” Kamm said.
However, even really good tests might only have 95% sensitivity, according to Kamm.
“No test is perfect,” she said.
The other factor in positive predictive value is the percentage of people with the disease.
A test with 95% sensitivity used on a population with half the people infected would have a positive predictive value of 90.5% — 90.5% of the positive results would be correct, and 9.5% would be false positives.
However, if only 5% of the population is infected, the same test would have a positive predictive value of 33.3%. Two-thirds of the positive results would be wrong.
“No matter what, we will have some people who test positive but do not have the disease,” Kamm said. “If the disease is not very common in the population, those false positives will be a bigger part of the positive test results.”
This is why health departments and hospitals only give tests to people with symptoms or who have been exposed to other known COVID-19 patients. Finding those exposed people is called contact tracing.
CONTACT TRACING
“Aggressive contact tracing and quarantining is a key containment method in pandemic preparedness,” Kamm said.
Contact tracing is about what it sounds like, tracking who a COVID-19 patient has had close contact with, typically by thoroughly interviewing them. Then, those contacted people are asked to self-quarantine and possibly to take a test for infection.
“By quarantining the contacts before they are infectious, we prevent them from interacting with other people, thus interrupting the chain of transmission in a community,” Kamm said.
Often, this can be done without disrupting life in the community as a whole, but with a new disease that may be infectious before symptoms are shown, authorities have implemented extra measures.