Poll: Some seniors skip COVID vaccine

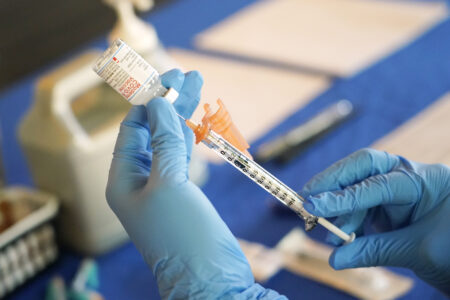
AP File photo A nurse prepares a syringe of a COVID-19 vaccine at an inoculation station in Jackson, Miss., July 19, 2022.
As Michigan sees growing rates of COVID-19 and high rates of influenza, a national poll led by the University of Michigan has found that 42% of individuals over 50 have not received a shot for either illness within the past six months.
In a survey of 2,964 adults over 50, 49% of individuals told the University of Michigan National Poll on Healthy Aging that it’d been more than a year since their last dose of the COVID-19 vaccine, while 15% never received the vaccine.
When asked why they hadn’t received an updated dose, the most common reason people gave was that they did not think they needed an updated dose.
Jeffrey Kullgren, a primary care physician at the VA Ann Arbor Healthcare System and the poll’s director, told Michigan Advance that while it’s good news that many older adults have been recently vaccinated against COVID-19 and influenza, many of the answers from individuals on why they didn’t receive the vaccine were in conflict with public health guidances.
That presents an opportunity for those adults and the clinicians who care for them to talk about what is known about the two vaccines, the patient’s risk for serious outcomes if they were to get sick and the ways they can reduce the risk if they do get sick, Kullgren said.
“For people in that age group, age 50 and older, you know, we would recommend that they receive those vaccines in order to reduce their risk for adverse outcomes,” Kullgren said. “But you know, that’s going to look a little different for each individual.”
While the largest share of individuals who had not received updated COVID-19 and influenza vaccines did not think they needed them, the second largest group cited concerns about potential side effects.
Addressing concerns about vaccine side effects can be a challenge for primary health care providers, Kullgren said, but helping patients to understand them is part of the job.
Additionally, with a wealth of information, both accurate and not, available online, it’s important to understand what patients are most concerned about, Kullgren said.
It can be difficult to know what people are referring to when they say they’re concerned about vaccine side effects, Kullgren said.
Whether it’s feeling poorly after receiving the flu vaccine – which is a sign that the vaccine is working – or dispelling concerns that don’t have any basis in scientific evidence, Kulgren maintains that it all starts with listening to the patient.
“At the margin, there may be some people that that makes a difference for them in their decision,” Kullgren said.
When looking at adults who did receive their updated vaccines versus those who didn’t, the poll found adults 75 and older, who carry the highest risk of hospitalization and death from both viruses, had the highest rate of uptake for the updated vaccines.
According to the poll, 46% of adults 75 and up had received a COVID-19 vaccine in the last six months, versus 37% of those ages 65 to 74 and 20% of those ages 50 to 64.
Adults over 50 who reported at least one chronic health condition were also more likely to have received recent flu and COVID-19 shots than those without any conditions. However, 39% of those with chronic health conditions said they hadn’t had either vaccine in the past six months.
“When we see people who are of more advanced age and people who have chronic conditions that have higher rates of vaccination, that’s a good thing, right?” Kullgren said. “Because they’re the people who are going to be at higher risk for having severe complications if they were to contract COVID-19 or influenza.”
As for why these individuals see higher rates of vaccination, Kullgren pointed to a few different factors.
“Are people sort of more attuned to health practices that may protect them from getting sicker, you know, or having other new, serious health issues? Probably.” Kullgren said.
Additionally, clinicians may also prioritize discussing the benefits of vaccination in the limited amount of time they have when meeting with patients.
“For these complex older patients or people with multiple chronic conditions, there are always more things to address than we have time for. And that’s just the unfortunate reality,” Kullgren said. “But we might make that a higher priority for somebody of advanced age who has a lot of chronic health problems.”
While the U.S. Food and Drug Administration and the Centers for Disease Control changed their recommendation on the COVID-19 vaccine last year; the National Poll on Healthy Aging saw little impact on COVID-19 vaccination rates as a result. According to the poll, less than 1% of individuals who chose not to receive the vaccine in the past year said they thought they were not eligible.
However, with the CDC recommending the vaccine for individuals ages 65 and older, the shift to a recommendation based on individual decision for those aged 6 months to 64 years old only impacts a fraction of the poll’s respondents.
During the rollout of the COVID-19 vaccine in 2021 and the years that followed, the idea that the individuals who are most at risk of illness were also the ones who received the most benefits has been diluted, Kullgren said. He encouraged both public health officials and individual providers to focus on that message when discussing the influenza and COVID-19 vaccines.
While it is always the patient’s choice at the end of the day, Kullgren said he always shares his concern for patients who are hesitant about the vaccines, but have risks for severe complications from either illness.
“I think coming from a place of concern and of benevolence, I think is important in this messaging at a time where many people continue to be distrustful of vaccines in general, and you know, these two vaccines in particular,” Kullgren said.